Depression is a common mental health issue that affects people of all ages. However, it often goes unnoticed and untreated in older adults. While aging naturally brings life changes—like retirement, health problems, or the loss of loved ones, depression is not a normal part of growing older. It’s a serious condition that can greatly lower a person’s quality of life if not treated.
In this guide, we’ll look at the warning signs of depression, the main causes, and the best treatment options for depression in older adults. We’ll also explain why early detection and the right kind of care are so important.
What Is Depression in Older Adults?
Depression in older adults is a serious mental health condition that affects the way someone thinks, feels, and lives day to day. It includes different types of mood disorders, from major depression to less severe but long-lasting types like dysthymia.
While depression can affect people at any age, it often appears differently in older patients than in younger adults.
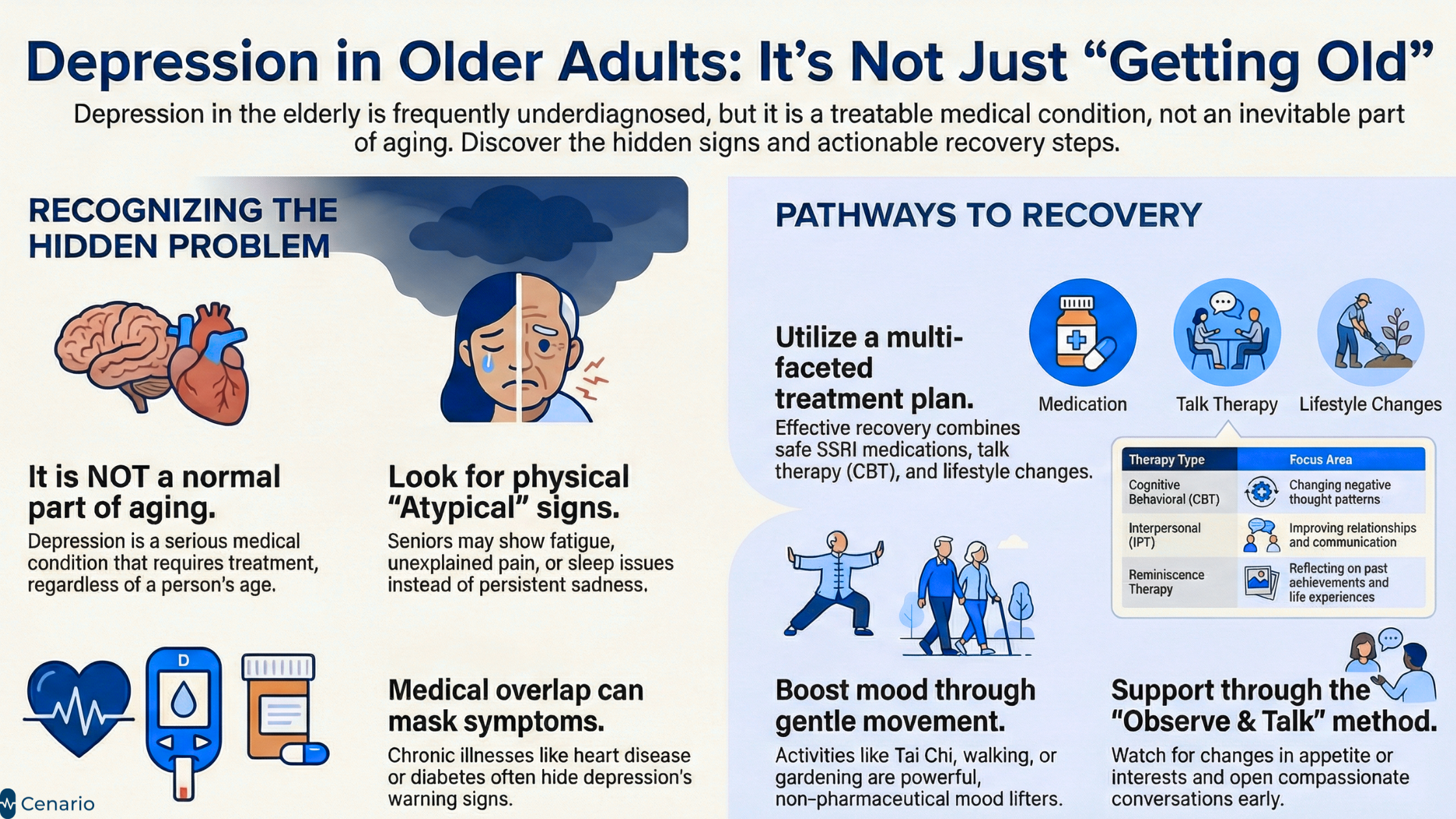
For example, younger people with depression often feel sad or hopeless and may talk about these feelings. But older adults may show different signs. They might have physical symptoms like tiredness, pain, or trouble sleeping. Or they may stop doing things they used to enjoy. Some may believe their feelings are just part of getting older or a natural response to grief or chronic illness.
But here’s the truth: Depression is not a normal part of aging. When it happens, it can harm a person’s health, make existing medical conditions worse, and reduce their ability to enjoy life.
The good news Depression is treatable. With the right antidepressant treatment, talk therapy, regular physical activity, and support from loved ones, older people can feel better and live full, healthy lives, even after depression has occurred.
Why Depression Is Often Missed in Older People
Despite its impact, depression in older adults is frequently underdiagnosed and undertreated. Several key reasons contribute to this:
1. Atypical Presentation of Symptoms
Depression in the elderly often doesn’t appear as persistent sadness. Instead, it may show up through non-specific physical symptoms, such as:
- Fatigue or low energy
- Slower movements or speech
- Body aches and pains
- Digestive issues
These may be misinterpreted as signs of physical illness or simply the effects of aging.
2. Overlap with Medical Illness
Many chronic illnesses, like diabetes, arthritis, heart disease, or Parkinson’s — share overlapping symptoms with depression, such as:
- Poor sleep
- Loss of appetite
- Reduced motivation
- Cognitive difficulties
As a result, depression may be mistakenly attributed to the underlying medical condition, causing the mood disorder to go unnoticed.
3. Stigma and Generational Attitudes
Older persons may come from a generation that sees mental illness as a weakness or moral failing. Because of this, they may:
- Avoid discussing their feelings
- Feel ashamed about seeking help
- Dismiss symptoms as “just being tired” or “getting old”
This stigma delays diagnosis and treatment.
4. Limited Access to Mental Health Care
Some older adults, particularly those who live alone, in rural areas, or in long-term care facilities — may not have regular visits with a mental health professional. Additionally, mobility issues, lack of transportation, or cognitive impairments may further limit access to care.
Common Symptoms of Depression in Older Adults
Understanding the symptoms of depression is essential for early intervention. These symptoms may be emotional, physical, or cognitive.
Emotional and Behavioral Signs:
- Persistent sadness or hopelessness
- Loss of interest in hobbies and social activities
- Irritability or agitation
- Feeling worthless or helpless
- Thoughts of death or suicide
Physical Signs:
- Changes in appetite or weight
- Sleep problems (insomnia or excessive sleep)
- Fatigue or slowed movements
- Unexplained pain or gastrointestinal issues
- Lack of energy or motivation
Cognitive Symptoms:
- Trouble concentrating
- Memory problems
- Confusion or indecisiveness
It’s important to note that developing depressive symptoms in older adults can sometimes mimic dementia or be misattributed to the natural aging process.
Major Causes of Depression in the Elderly
Depression does not occur in a vacuum. It is often the result of interacting psychological, biological, and environmental factors.
1. Chronic Medical Conditions
Conditions such as heart disease, diabetes, stroke, arthritis, Parkinson’s disease, and cancer are strongly associated with depression in older adults. Living with chronic illness can be emotionally and physically exhausting, especially when pain, limited mobility, or disability are involved.
2. Medication Side Effects
Some medications commonly prescribed to older patients may cause depressive symptoms. For example, beta-blockers, corticosteroids, benzodiazepines, and even some pain medications may lead to mood changes or fatigue.
3. Loss and Grief
The loss of a spouse, friends, or even independence can trigger grief that sometimes transitions into clinical depression. Grief is natural, but when depression occurred for more than two weeks and impairs function, it requires professional attention.
4. Social Isolation
Many elderly individuals experience isolation due to reduced mobility, retirement, or the deaths of peers. Lack of social contact is a major contributor to developing depressive symptoms in older persons.
5. Cognitive Decline and Dementia
Depression can both mimic and coexist with dementia. Seniors with Alzheimer’s or other types of cognitive decline are more susceptible to depression, which complicates diagnosis and treatment.
The Role of Physical Activity in Managing Depression
Regular physical activity is one of the most effective, non-pharmaceutical methods to prevent and manage symptoms of depression in seniors. It can improve mood, enhance cognitive function, promote better sleep, and reduce stress.
Types of recommended physical activity include:
- Brisk walking
- Water aerobics
- Tai chi or yoga
- Gardening or light chores
- Chair exercises for those with mobility issues
Even modest increases in movement can lead to measurable improvements in mental health, particularly for those with chronic illness.
Diagnosis: When to Seek Help
If you or someone you love shows signs of emotional withdrawal, hopelessness, or a notable change in daily functioning, it’s crucial to consult a mental health professional. Tools like the Geriatric Depression Scale (GDS) can aid in screening, and a thorough evaluation by a physician can rule out other medical conditions.
Treatment of Depression in Older Adults
Treatment of depression in seniors is multi-faceted and should be personalized to the individual’s health, history, and preferences.
1. Antidepressant Treatment
Medications such as Selective Serotonin Reuptake Inhibitors (SSRIs) e.g., sertraline, escitalopram, are often prescribed. These have fewer side effects and are considered safer for older patients compared to older drug classes like tricyclic antidepressants.
However, doctors must monitor for potential interactions with other medications being taken for medical illness or physical illness.
2. Psychotherapy
- Cognitive Behavioral Therapy (CBT) helps patients recognize and change negative thought patterns.
- Interpersonal Therapy (IPT) focuses on improving relationships and communication.
- Reminiscence therapy encourages reflection on past achievements and experiences.
Talk therapy is highly effective, especially when combined with medication.
3. Lifestyle Interventions
- Improved diet and nutrition
- Better sleep hygiene
- Daily routines and structured activities
- Community engagement and volunteer work
Encouraging meaningful daily activity and social interaction plays a major role in recovery.
4. Electroconvulsive Therapy (ECT)
For older patients with severe or treatment-resistant depression, Electroconvulsive Therapy (ECT) can be a life-saving intervention. ECT is particularly effective when depression includes suicidal ideation, psychosis, or when rapid response is needed.
Although once controversial, modern ECT is safe, performed under anesthesia, and has proven effective in elderly populations.
Supporting a Loved One Through Depression
Family members and caregivers are crucial in identifying signs of depression and encouraging treatment. Here’s how you can help:
- Observe: Watch for changes in mood, appetite, sleep, or interest in activities.
- Talk: Open the conversation with compassion and patience.
- Assist: Help schedule appointments and accompany them to the doctor.
- Support: Offer emotional support and reduce isolation.
- Educate: Learn about depression to reduce stigma and improve understanding.
Conclusion: Hope and Healing Are Possible
Depression in older adults is a treatable medical condition, not an inevitable part of aging. No one should have to endure silent suffering, especially when effective help is available. With the right combination of antidepressant treatment, psychotherapy, physical activity, and strong social support, older persons can recover, regain joy, and live vibrant, meaningful lives well into their later years.
If you or someone you care about is showing symptoms of depression, don’t ignore the signs. Early intervention makes a profound difference.
Take Action Now
Take our quick quiz to receive a personalized supplement recommendation designed to support mood, brain health, and emotional well-being, tailored specifically for older adults.
Take the Quiz Now and discover natural options that complement your depression care plan.
Because mental health matters at every age, and every step toward healing counts.
Frequently Asked Questions
1. Is depression a normal part of aging?
No, depression is not a normal or inevitable part of aging. While older people may face challenges such as loss, health issues, or social isolation, these do not automatically lead to depression. If symptoms of depression persist for more than two weeks and interfere with daily life, it’s important to seek help from a mental health professional.
2. Can physical illness or chronic conditions cause depression in older adults?
Yes. Chronic illness and other medical conditions are significant risk factors for developing depressive symptoms. Conditions like arthritis, diabetes, cancer, and cardiovascular disease can impact mood and overall well-being. Additionally, certain medications used to treat these conditions can have side effects that contribute to depression. Treating the underlying medical illness alongside depression often leads to better outcomes.
3. What is the best treatment for depression in elderly patients?
The best treatment for depression in older patients usually involves a comprehensive approach, including:
- Antidepressant treatment (with careful monitoring for side effects)
- Psychotherapy, such as Cognitive Behavioral Therapy (CBT)
- Physical activity to boost mood and energy levels
- In severe or treatment-resistant cases, Electroconvulsive Therapy (ECT) may be considered
Each treatment plan should be tailored to the individual’s health status, preferences, and lifestyle.
4. How can family members help an older loved one dealing with depression?
Family members can help by recognizing signs like low mood, fatigue, or withdrawal, and starting a kind, supportive conversation. Encouraging professional help, supporting treatment, and staying socially connected with their loved one can make a big difference in recovery.







