When people hear the word hallucinations, they often think of psychotic disorders like schizophrenia. However, many people with post traumatic stress disorder (PTSD) also report sensory experiences such as hearing or seeing things that aren’t there. This leads to the important and often overlooked question: Can post traumatic stress disorder cause hallucinations?
Recent research suggests that for some individuals, especially those with a history of severe traumatic experiences or childhood trauma, the answer is yes. People with traumatic stress disorder PTSD may experience hallucinations, particularly auditory hallucinations and visual hallucinations—that are linked to their trauma history.
Let’s explore how PTSD affects the brain, why hallucinations may occur, and what treatment options exist for managing symptoms effectively.
Post traumatic stress disorder (PTSD) is a mental health condition that can develop after a person is exposed to a traumatic event that involves real or perceived danger. This could include physical or sexual assault, military combat, serious accidents, natural disasters, or a life‑threatening illness. Childhood trauma is especially important, because early trauma can affect brain development and increase the risk of long‑lasting symptoms later in life.
PTSD does not mean someone is “weak” or unable to cope. It is the brain’s response to overwhelming stress. After trauma, the brain may stay in survival mode, constantly scanning for threats, even when the danger is gone.
Core Symptoms of PTSD
The symptoms of PTSD are grouped into four main categories:
1. Intrusive Memories
These are unwanted memories of the trauma that force themselves into awareness. They may include:
- Flashbacks that feel like the event is happening again
- Nightmares related to the trauma
- Disturbing thoughts or images that appear suddenly
These memories can be very vivid and emotional, making it hard to stay focused on the present.
2. Avoidance
People with PTSD often try to avoid anything that reminds them of the traumatic experience. This can include:
- Avoiding places, people, or activities linked to the trauma
- Avoiding thoughts or conversations about what happened
Avoidance can shrink a person’s world over time and interfere with relationships or daily responsibilities.
3. Negative Symptoms
These symptoms involve changes in mood, thinking, and emotional connection. Examples include:
- Persistent guilt, shame, or blame
- Feeling emotionally numb or detached from others
- Difficulty feeling joy or positive emotions
- Negative beliefs about oneself or the world
These negative symptoms can strongly affect self‑esteem and mental health.
4. Hyperarousal
Hyperarousal means the body remains in a state of high alert. Symptoms may include:
- Being easily startled or jumpy
- Irritability or angry outbursts
- Trouble sleeping or concentrating
- Constant feeling of danger
Together, these symptoms can last for months or years and often interfere with work, relationships, and overall quality of life.
What Are Hallucinations?
Hallucinations are sensory experiences that feel real but occur without an external stimulus. In other words, the brain creates a perception even though nothing outside the body is causing it.
Hallucinations can affect any of the five senses:
Auditory Hallucinations
These involve hearing sounds that others cannot hear, such as:
- Voices speaking, whispering, or yelling
- Sounds like footsteps, knocking, or crying
- Trauma‑related phrases or threats
Visual Hallucinations
These involve seeing things that are not actually present, including:
- Images, shadows, or figures
- Brief flashes of scenes
- Detailed visuals connected to past trauma
Other Sensory Hallucinations
Less commonly, people may experience:
- Smelling odors that are not there
- Feeling touch or pressure with no physical cause
- Tasting something without eating or drinking
Hallucinations and PTSD
Although hallucinations are often associated with psychotic disorders, research shows they can also occur in people with post traumatic stress disorder, especially those with severe trauma or childhood trauma.
In PTSD, hallucinations are usually trauma‑related. They often reflect memories or sensory fragments from the original traumatic event. For example:
- Hearing the voice of an abuser
- Seeing a traumatic scene replay briefly
- Experiencing sounds, smells, or sensations tied to the trauma
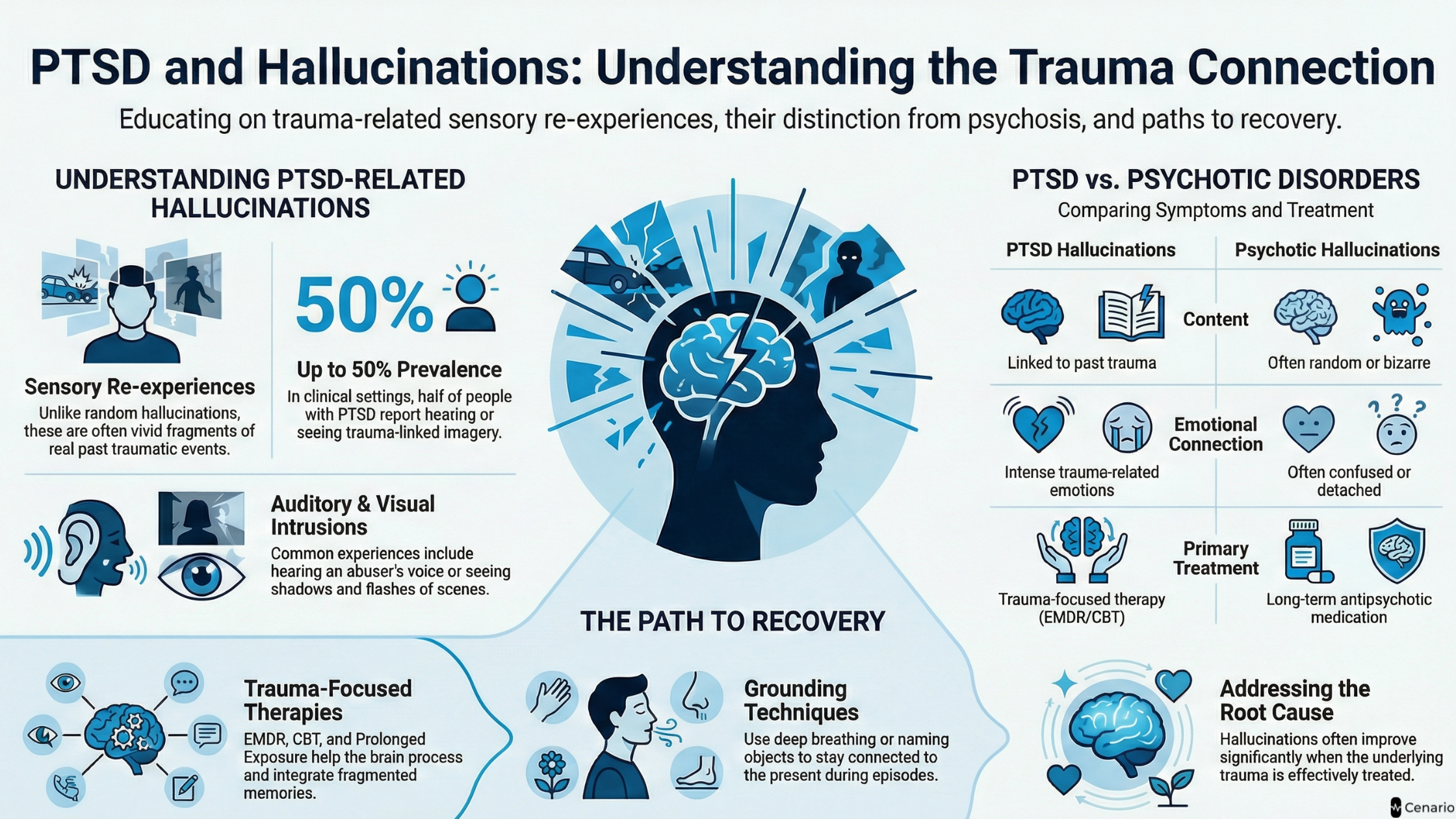
These hallucinations are different from those seen in psychotic disorders because they are closely linked to real past experiences rather than unrelated or bizarre beliefs.
Understanding this distinction is important, because PTSD‑related hallucinations often improve when the underlying trauma is treated, especially with trauma‑focused therapies.
How Can PTSD Cause Hallucinations?
So, can post traumatic stress disorder cause hallucinations? Yes—many people with traumatic stress disorder PTSD report auditory hallucinations, visual hallucinations, or other sensory experiences that seem connected to their past trauma.
1. Trauma-Related Intrusions
People with PTSD may hear a voice that sounds like their abuser or see a traumatic scene replay in front of them. These are not random. They are often trauma-related hallucinations, meaning they are connected to real-life memories of the traumatic event.
These experiences may feel different from classic hallucinations seen in schizophrenia. In PTSD, hallucinations often match the trauma and feel like an overwhelming flashback, creating a sense that the traumatic event is happening all over again.
2. Dissociation and Memory Fragmentation
During a traumatic experience, especially one involving childhood trauma, the brain may become overwhelmed and dissociate, a defense mechanism where the mind separates itself from the event to survive. This can cause the memory to be stored in fragments.
Later, these fragmented memories may resurface as hallucinations in PTSD. For example, someone might suddenly smell smoke or hear screaming with no actual source. These sensory experiences can be terrifying and very real to the person experiencing them.
Brain Changes Linked to PTSD Hallucinations
PTSD affects brain regions responsible for memory, perception, and emotional regulation:
- The amygdala, which processes fear, becomes hyperactive—putting the brain in constant alert.
- The hippocampus, which helps form and organize memories, may shrink or function poorly after trauma.
- The prefrontal cortex, which helps with reasoning and controlling emotions, may become less active, making it harder to distinguish between memory and reality.
Together, these brain changes contribute to intrusive memories, distorted perception, and trauma-related hallucinations.
Predictive Coding and Perception Errors
One scientific theory, called predictive coding, helps explain why people with PTSD may experience hallucinations. According to this model, the brain constantly predicts what it expects to perceive based on past experiences. After trauma, these predictions can become overly focused on danger and threat.
As a result, the brain might “fill in” sensory gaps with trauma-related content—leading to auditory or visual hallucinations, even when no external danger is present.
How Are PTSD Hallucinations Different from Psychosis?
Although both involve hallucinations, PTSD and psychotic disorders differ in several key ways:
| Feature | PTSD | Psychotic Disorders |
|---|---|---|
| Content of Hallucinations | Usually linked to past trauma | Often unrelated to trauma |
| Belief System | Person may know it’s from past | May involve delusions |
| Emotional Reaction | Strong emotional connection to trauma | Often confused or bizarre content |
| Treatment Response | Often improves with trauma therapy | May require long-term antipsychotics |
These differences are important for proper diagnosis and treatment planning.
Treatment Options for PTSD Hallucinations
1. Trauma-Focused Psychotherapies
The most effective treatment for hallucinations in PTSD is trauma-focused therapy, not antipsychotic medication. Evidence-based approaches include:
- Cognitive Behavioral Therapy (CBT) – Helps people change harmful thought patterns related to the trauma.
- Prolonged Exposure Therapy – Involves safely revisiting traumatic memories to reduce fear and avoidance.
- Eye Movement Desensitization and Reprocessing (EMDR) – Uses eye movements or tapping to help process traumatic memories and reduce emotional intensity.
These therapies help people re-integrate fragmented memories and create a sense of safety and control.
2. Medications
While therapy is the first-line treatment, medications may help with managing symptoms like anxiety, depression, or severe sleep issues. These may include:
- SSRIs (Selective Serotonin Reuptake Inhibitors) – Often prescribed for core symptoms of PTSD.
- Antipsychotics – Sometimes used for auditory or visual hallucinations, though they are not always effective for trauma-related symptoms and may have side effects.
Medication is typically used alongside, not instead of, trauma-focused therapy.
Living with PTSD and Hallucinations: What to Do
If you or someone you know is experiencing hallucinations in PTSD, here are steps you can take:
- Seek a professional evaluation to understand whether the hallucinations are trauma-based or due to another condition.
- Keep a journal of sensory experiences, triggers, and times they occur.
- Practice grounding techniques like deep breathing, cold water, or naming objects in the room to stay connected to the present.
- Get enough sleep and avoid drugs or alcohol, which can worsen hallucinations.
- Explore trauma therapy, such as CBT, EMDR, or prolonged exposure therapy, with a licensed therapist.
Final Thoughts: Can PTSD Cause Hallucinations?
The short answer is yes, post traumatic stress disorder can cause hallucinations, especially in individuals with a history of childhood trauma or severe traumatic experiences. These sensory experiences often mirror the content of the trauma and differ significantly from those seen in psychotic disorders.
Understanding and addressing the root trauma is key to managing symptoms. With the right treatment, especially cognitive behavioral therapy, EMDR, and other trauma-focused methods—many people see dramatic improvements. If you’re struggling, know that help is available and healing is possible.
Looking for natural support on your healing journey?
Take the cenario quiz to get a personalized supplement recommendation based on your mental health profile, symptoms, and wellness goals.
Frequently Asked Questions (FAQs)
1. Are hallucinations common in post traumatic stress disorder (PTSD)?
Hallucinations are not one of the main symptoms used to diagnose PTSD, but many people with PTSD do report them, especially auditory hallucinations (like hearing voices) and visual hallucinations (like seeing images or shadows). Research shows that in some clinical settings, up to 50% of people with PTSD may experience hallucinations related to their trauma.
2. Can childhood trauma lead to hallucinations later in life?
Yes. Childhood trauma is a major risk factor for developing post traumatic stress disorder. It can also increase the chances of experiencing hallucinations in PTSD as an adult. Early trauma can affect how the brain develops, especially parts like the prefrontal cortex and hippocampus, which are important for memory and how we understand what’s real or not.
3. How do doctors tell the difference between flashbacks and hallucinations in PTSD?
Doctors look at what the person is experiencing and when it happens. Flashbacks usually happen when something reminds the person of their trauma. They often involve intrusive memories that feel like the trauma is happening again. Hallucinations, on the other hand, can happen without any trigger and are usually sensory experiences (like hearing or seeing something that isn’t there). Both can happen in PTSD but may need different treatment approaches.
4. What is the best way to treat hallucinations in PTSD?
The best way to treat hallucinations in PTSD is to focus on healing the trauma itself. Trauma-focused therapies, such as cognitive behavioral therapy (CBT), prolonged exposure therapy, and eye movement desensitization and reprocessing (EMDR)—help people process their traumatic memories and reduce symptoms. Medication may also help with related problems like anxiety or trouble sleeping, but therapy is usually the most important part of treatment.







