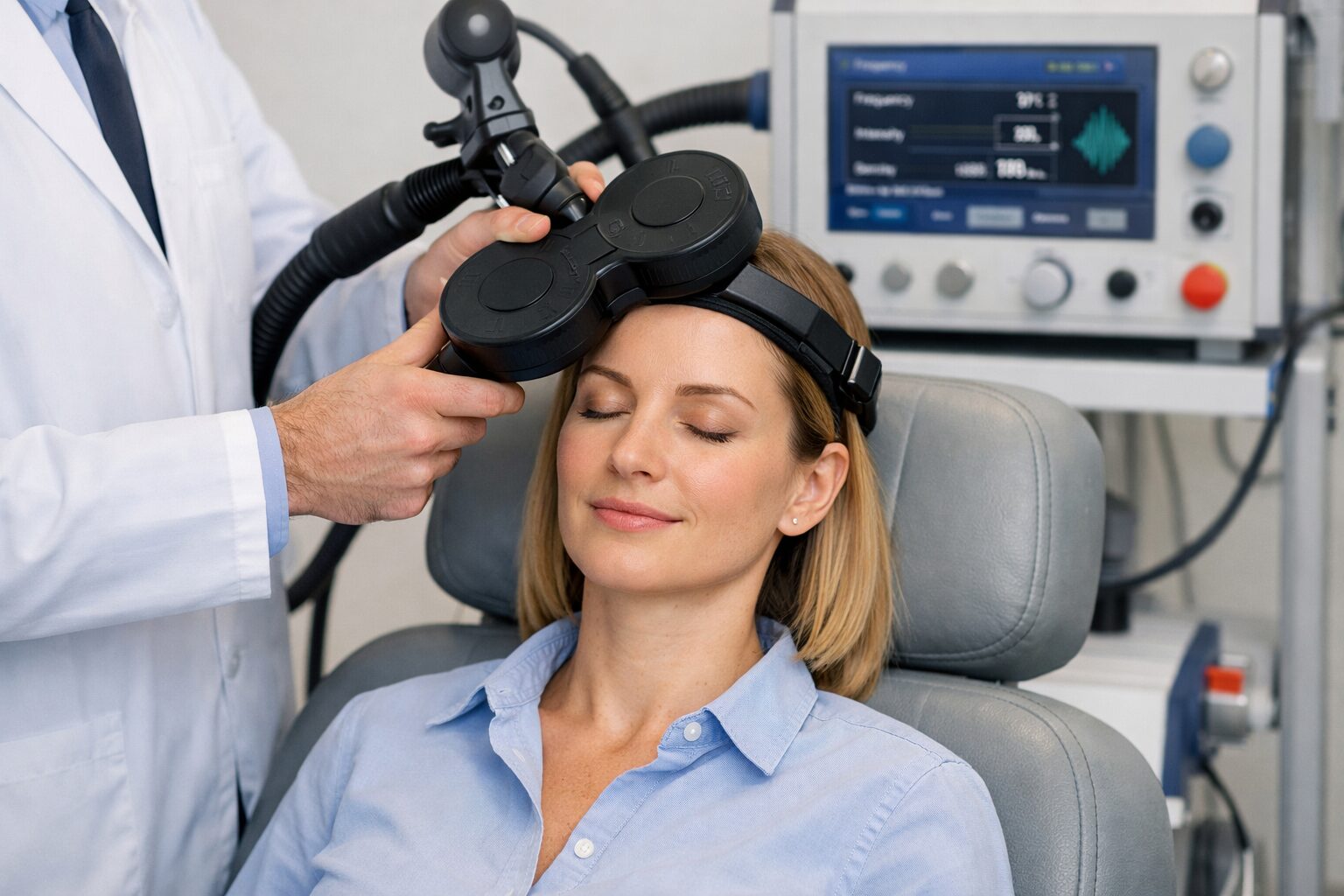
Introduction to transcranial magnetic stimulation TMS
Transcranial magnetic stimulation TMS is changing how clinicians and patients think about treating major depression. It is a noninvasive form of brain stimulation that uses magnetic pulses to influence nerve cells linked to mood regulation. For people whose symptoms have not improved with antidepressants or therapy, transcranial magnetic stimulation tms offers a different pathway that targets the brain without surgery or systemic medication effects.
Why clinicians and patients are paying attention
Transcranial magnetic stimulation tms attracts attention for several practical reasons. It does not require anesthesia. It avoids systemic side effects commonly associated with oral antidepressants. Many people describe the appeal as a targeted option that works directly on brain circuits linked to mood. As evidence accumulates, more providers offer TMS and more patients ask about it when standard treatments fall short.
Approved uses and expanding research
While major depression is the primary, FDA‑approved use, transcranial magnetic stimulation tms is being studied for obsessive compulsive disorder, certain types of migraine, and smoking cessation. Researchers are also investigating applications in anxiety, PTSD, stroke recovery, and neurological conditions. That growing research base is why TMS appears more often in clinical practice and media coverage.
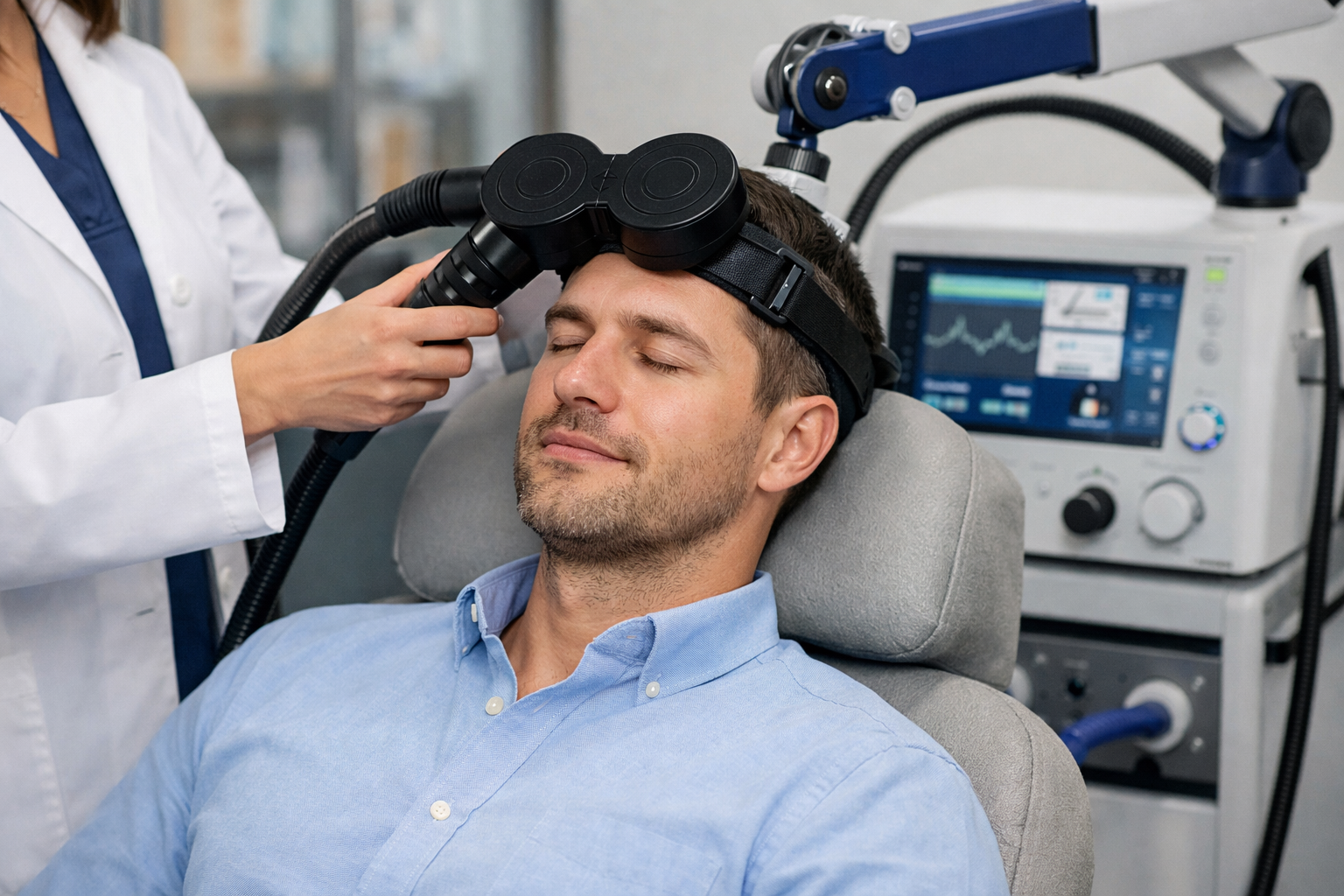
If you are exploring whether transcranial magnetic stimulation tms might be relevant for you or a loved one, the next sections will examine how it works, what outcomes patients can expect, and practical steps for getting evaluated.
How TMS works
Transcranial magnetic stimulation tms delivers brief magnetic pulses through a coil placed on the scalp to influence electrical activity in targeted brain circuits. Clinicians locate a motor hotspot and measure a motor threshold to set individualized dose. Most treatment centers use repetitive protocols, either high‑frequency rTMS or patterned approaches such as theta burst, to promote lasting changes in neural connectivity and plasticity.
The goal with transcranial magnetic stimulation tms is to modulate underactive or overactive regions involved in mood and cognition. Repeated pulses encourage synaptic strengthening and network rebalancing rather than producing a seizure. That mechanism helps explain why effects accrue over days to weeks rather than appearing instantly.
Effectiveness and safety
Large clinical series and randomized trials report roughly a 60% response rate for treatment‑resistant depression and sustained benefit for many patients at six months. Transcranial magnetic stimulation tms has shown durable remission in a substantial subset when paired with follow up or booster sessions.
Safety is generally favorable. The most common complaints are scalp discomfort and transient headaches that improve with simple analgesics. Rare but serious events include seizure, with risk estimated at less than one in a few thousand treatments when screening and protocols are followed. Hearing protection is standard during sessions because coil clicks can be loud.
Compared with electroconvulsive therapy, transcranial magnetic stimulation tms does not require general anesthesia and has far fewer cognitive side effects. That difference makes it an attractive option for patients who cannot tolerate medication side effects or who want a noninvasive neuromodulation option.
Applications beyond depression
Clinicians and researchers are expanding uses for transcranial magnetic stimulation tms. Current approved and evidence‑supported areas include:
- FDA‑approved indications beyond major depression, where applicable in practice settings.
- Obsessive compulsive disorder and certain migraine types, with structured protocols demonstrating benefit.
- Off‑label but promising applications such as PTSD, anxiety disorders, stroke rehabilitation, Parkinson’s motor symptoms, chronic pain modulation, and smoking cessation support.
Trials continue for Alzheimer’s disease and neurodevelopmental conditions, but those remain experimental and should be pursued only in research settings.
What to expect during treatment
A typical transcranial magnetic stimulation tms course involves five sessions per week for four to six weeks, followed by occasional booster visits. Each session usually lasts 20 to 40 minutes after setup. The initial visit includes mapping and threshold testing; subsequent sessions require sitting upright while the device delivers pulses over the targeted area.
Patients remain alert and can return to most daily activities immediately. Many report a tapping sensation and mild scalp ache during early sessions. Clinical improvement often begins after two to four weeks, though individual timelines vary. If symptoms do not respond, clinicians may adjust coil placement, pulse parameters, or consider alternative therapies.
Cost, insurance, and practical access
Cost varies by region and protocol, and full courses commonly range from several thousand to over ten thousand currency units in markets without coverage. Most private insurers and many public plans provide reimbursement for transcranial magnetic stimulation tms when documentation shows prior failed medication trials and clinical necessity. Prior authorization is typical, and providers usually submit treatment notes and outcome measures to secure coverage.
Practical steps before scheduling include an evaluation by a qualified clinician, verification of insurance benefits, and planning for the time commitment.
If you are considering transcranial magnetic stimulation tms, discuss realistic goals, expected timelines, and insurance steps with your clinician. Clear planning improves access and sets appropriate expectations for outcomes and ongoing care.
Practical considerations and patient journey
When you decide to pursue transcranial magnetic stimulation tms, planning makes the process smoother. Most programs begin with a clinical evaluation that reviews your psychiatric history, prior medication trials, and any medical issues that could affect treatment. Expect a baseline assessment that often includes symptom scales such as PHQ‑9 and a focused safety screen for seizure risk and implants.
The first in‑clinic visit typically includes mapping to identify stimulation targets and determine the motor threshold. That visit may take 60 to 90 minutes. Follow up sessions are shorter. Patients usually sit in a recliner while the coil delivers pulses and may read, listen to music with provided hearing protection, or work on a laptop if positioned for comfort.
Scheduling is one of the biggest practical hurdles. Standard courses involve frequent visits over several weeks. Many centers offer early morning, evening, or condensed accelerated options to help patients keep work or family commitments. Ask your clinic about flexible scheduling and whether remote check ins are available for progress tracking.
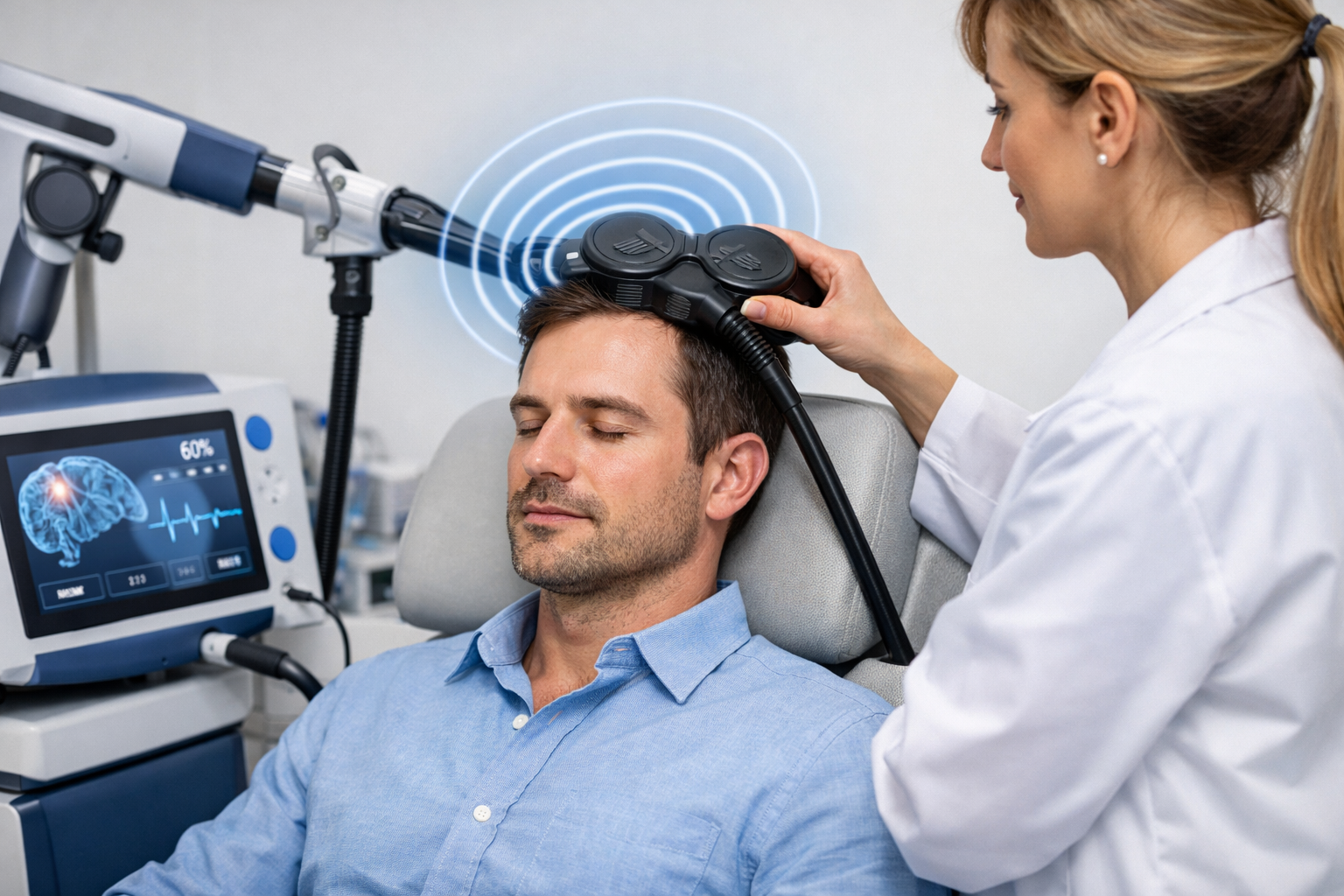
Preparing for treatment and daily logistics
Before each session, plan to arrive a few minutes early for check‑in. Wear comfortable clothing and avoid hair products that interfere with coil placement. Bring documentation your insurer may request and a list of current medications. If you rely on public transit or need parking, confirm options ahead of time to minimize delays.
Transport and caregiving are common concerns. Because patients are alert after transcranial magnetic stimulation tms, driving is usually permitted unless your clinician advises otherwise for individual reasons. If you are unsure, arrange transportation for the first sessions while you gauge how you feel.
Tracking progress and maintenance plans
Clinicians will monitor symptoms regularly and may use standardized questionnaires to document response. If you show partial improvement, options include continuing the initial course, adjusting stimulation parameters, or adding booster sessions. Booster schedules vary by clinic and may be monthly or triggered by symptom recurrence.
Long term care often combines transcranial magnetic stimulation tms with ongoing medication management, psychotherapy, and lifestyle strategies. A clear relapse prevention plan and access to follow up care improve the likelihood of sustained benefit.
Cost and insurance navigation
Costs for transcranial magnetic stimulation tms vary widely by geography, device, and treatment intensity. In markets without coverage, full courses commonly range from several thousand to over ten thousand in local currency. When insurance is involved, prior authorization is usually required and clinics commonly provide documentation of prior medication trials and objective outcome measures.
If a claim is denied, options include an internal appeal, payment plans offered by clinics, manufacturer financing, or enrollment in research trials. Before scheduling, request a benefits check and an estimate of expected out of pocket expenses so you can compare choices and avoid surprises.
When TMS is not the final step
If transcranial magnetic stimulation tms does not provide adequate relief, clinicians review options such as optimizing medication regimens, considering electroconvulsive therapy, exploring ketamine or esketamine treatments, or referring to clinical trials. The key is an individualized plan with measured goals and timely reassessment.
Final thoughts and next steps
Transcranial magnetic stimulation tms is a practical, evidence‑based option for many patients who need an alternative to medication and psychotherapy alone. If you are evaluating TMS, use structured tools, get a thorough clinical assessment, and confirm insurance details before committing to a full course.
If you think transcranial magnetic stimulation tms might help, contact a qualified provider to discuss realistic goals, timeline, and insurance steps. Early planning and clear expectations increase your chances of a successful treatment experience.
Looking for the best option is pointless if it is not right for you.
Take the Cenario Quiz and get a personalized, science-backed recommendation in under 3 minutes.
Frequently Asked Questions
How soon will I notice benefits after starting transcranial magnetic stimulation tms?
Some people notice changes within two to four weeks, but for most meaningful improvements it takes the full course. Clinicians use symptom scales during transcranial magnetic stimulation tms to track gradual progress and guide adjustments.
Can people with metal implants receive transcranial magnetic stimulation tms?
Metal implants near the head or electronic implants such as certain pacemakers may pose a contraindication. A full safety screen is required because transcranial magnetic stimulation tms can interact with metallic or electronic devices in or near the skull.
Will my insurance cover transcranial magnetic stimulation tms?
Many private and some public plans cover transcranial magnetic stimulation tms for treatment resistant depression with prior authorization, but coverage rules vary. Ask your clinic to submit a benefits check and prepare documentation of prior treatments to improve approval chances.
.