Electroconvulsive Therapy (ECT) is a highly effective and medically approved treatment used to address severe mental illnesses, especially when people do not respond to other treatments like antidepressant medications or psychotherapy. Despite lingering misconceptions, ECT is a safe and carefully controlled procedure that has helped thousands of individuals manage conditions such as bipolar disorder, treatment-resistant depression, schizophrenia, and catatonia.
This blog explores the benefits of ECT, how it works, the ECT procedure, and common concerns such as side effects, memory loss, and the role of general anesthesia and muscle relaxants during treatment.
What Is Electroconvulsive Therapy (ECT)?
Electroconvulsive Therapy (ECT) is a medical procedure in which small electrical currents are passed through the brain to intentionally trigger a brief, controlled seizure. This seizure is believed to create changes in brain chemistry that can significantly improve the symptoms of certain mental health conditions.
ECT is primarily used when other effective treatments, such as medications or therapy, haven’t worked or when symptoms are severe and require rapid relief, like in the case of suicidal thoughts, extreme mood swings, or psychotic behavior.
Mental Health Conditions Treated with ECT
ECT is used to treat several severe psychiatric conditions, especially when they are treatment-resistant or life-threatening. Common conditions include:
- Treatment-resistant depression
- Bipolar disorder (especially during manic or depressive episodes)
- Schizophrenia (with symptoms like hallucinations or delusions)
- Catatonia (a state of abnormal movement or speech)
- Severe postpartum depression
- Suicidal ideation requiring fast relief
Key Benefits of Electroconvulsive Therapy (ECT)
1. Rapid Relief of Severe Symptoms
One of the most important benefits of ECT is its ability to quickly relieve intense symptoms of mental illnesses, especially treatment-resistant depression. Many patients begin to experience improvements after just a few sessions, which is much faster than most antidepressant medications, which may take several weeks to work.
In cases involving suicidal ideation or refusal to eat, ECT treatment can literally be life-saving by providing highly effective symptom relief within days.
2. Effective When Other Treatments Fail
ECT is especially helpful for people who do not respond to other treatments, including medications and psychotherapy. It is often considered a “last resort” for treatment-resistant depression, but research shows that many patients who undergo ECT experience significant improvements when nothing else has worked.
3. Safe and Controlled Medical Procedure
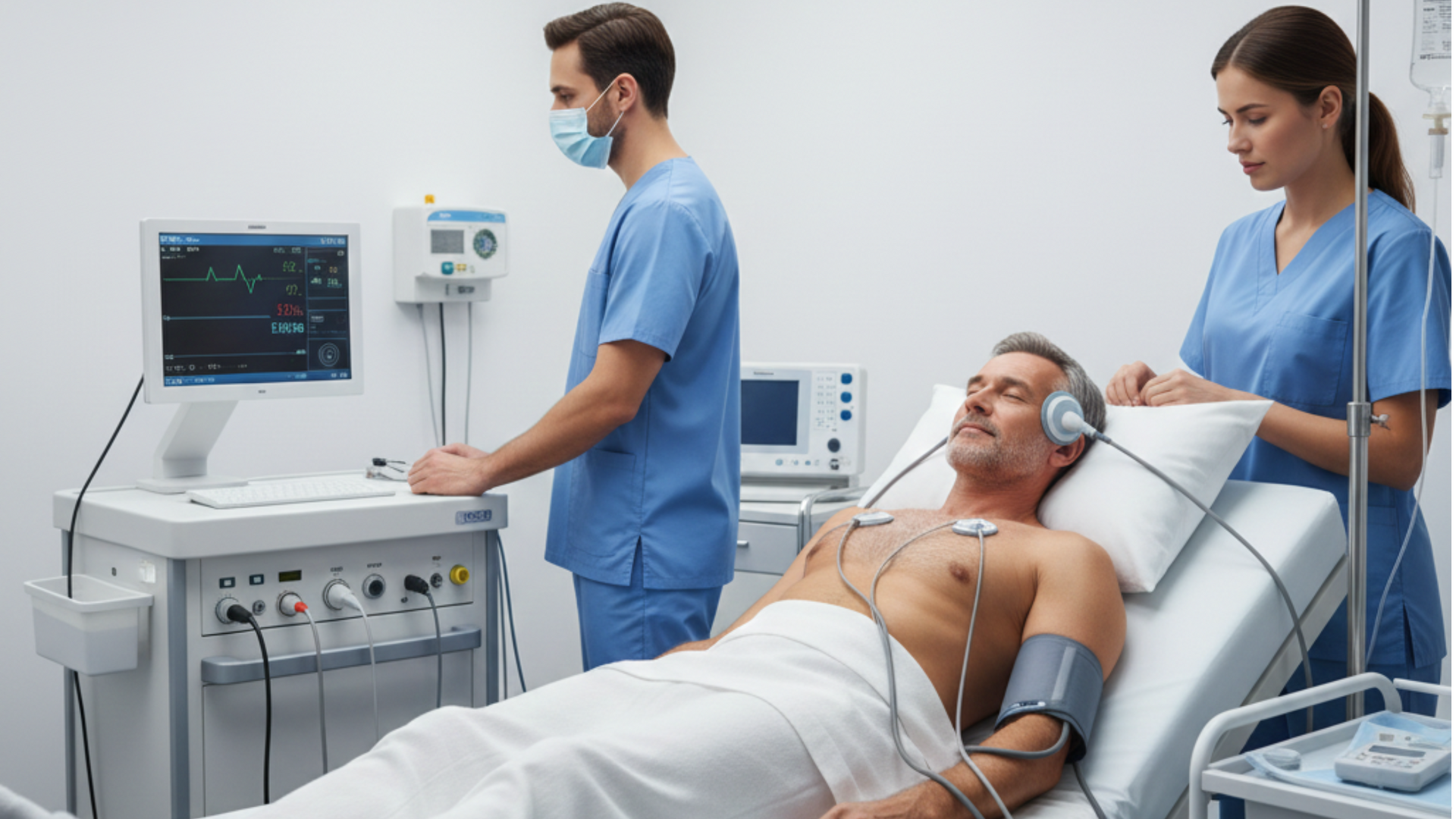
Modern ECT procedures are conducted in hospitals under strict medical supervision. Patients are given general anesthesia to ensure they are unconscious and feel no pain. A muscle relaxant is also administered to minimize physical movement during the seizure and prevent injury.
Vital signs, including blood pressure, heart rate, and oxygen levels, are closely monitored throughout the procedure.
4. Minimal and Manageable Side Effects
While side effects are a concern for many people considering ECT, the reality is that most effects are mild and temporary. The most common side effect is short-term memory loss, especially around the time of the treatment. Some people may also experience confusion after waking up from the procedure, but this usually fades within an hour.
Long-term memory loss is rare, and serious complications are extremely uncommon when ECT is administered by trained professionals.
5. Improved Quality of Life
By reducing the symptoms of certain mental health conditions, ECT allows individuals to return to their everyday lives. Many people report improvements in mood, energy, motivation, and social relationships. They often find themselves better able to work, go to school, maintain relationships, and enjoy life.
When successful, ECT doesn’t just treat symptoms, it restores hope and functionality.
What to Expect During the ECT Procedure
Here’s a breakdown of what happens when a person undergoes ECT:
Before the Procedure:
- A full medical and psychiatric evaluation is conducted.
- The patient gives informed consent.
- Medications may be adjusted or paused as directed.
During the Procedure:
- The patient is given general anesthesia and a muscle relaxant.
- Electrodes are placed on the scalp (either on one side or both).
- A brief, controlled electrical pulse induces a seizure lasting 30–60 seconds.
- Blood pressure, heart rate, and breathing are monitored the entire time.
After the Procedure:
- The patient wakes up in a recovery area within 15–20 minutes.
- Mild confusion or headache may occur but usually resolves quickly.
- Most people resume normal activities within a few hours.
How Often is ECT Given?
A full course of ECT treatment typically involves 6 to 12 sessions, given 2–3 times per week. Some individuals may require maintenance ECT sessions on a monthly basis to prevent relapse, especially in chronic or recurrent cases.
Addressing Concerns About Memory Loss and Side Effects
The topic of memory loss is often discussed in relation to ECT. Most memory problems are short-term and affect only the period immediately before or after treatment. It’s important to understand that:
- Memory typically improves once ECT sessions are completed.
- Serious long-term memory loss is rare.
- Doctors always balance the benefits and risks for each patient.
Other side effects may include temporary confusion, muscle aches, headache, or nausea—but these are generally mild and resolve quickly.
Is ECT Right for You?
ECT is not the first-line treatment for most mental health conditions, but for those with severe, treatment-resistant depression or other serious psychiatric symptoms, it can be life-changing. The decision to pursue ECT is made after careful evaluation and consultation between the patient, their family, and their healthcare providers.
If you or a loved one is struggling with a severe mental health condition and hasn’t improved with medications or therapy, it may be worth exploring the benefits of electroconvulsive therapy.
Final Thoughts: Why ECT Remains a Powerful Option
Despite decades of controversy and stigma, ECT treatment has evolved into a safe, effective, and compassionate form of care. Thanks to advances in medical science, like the use of general anesthesia, muscle relaxants, and strict safety protocols patients can now undergo ECT in a controlled environment and recover quickly.
ECT remains one of the most highly effective options for managing severe mental illnesses, particularly when other treatments haven’t worked. Whether you’re dealing with bipolar disorder, treatment-resistant depression, or another serious mental health condition, learning about the benefits of ECT can be the first step toward healing and long-term wellness.
As you explore your mental health options, it’s also important to support your body and mind holistically. Take our quick quiz to get a personalized supplement recommendation based on your individual needs and wellness goals. It’s a simple way to complement your treatment journey with targeted support.
Frequently Asked Questions (FAQs)
Frequently Asked Questions (FAQs)
1. Is Electroconvulsive Therapy (ECT) safe?
Yes, modern electroconvulsive therapy (ECT) is a safe and medically supervised procedure. It is performed under general anesthesia with constant monitoring of vital signs such as blood pressure and heart rate. While some side effects like confusion or short-term memory loss can occur, serious complications are very rare.
2. Does ECT cause permanent memory loss?
Most people experience short-term memory loss during or shortly after ECT treatment, particularly around the time of the procedure. In rare cases, long-term memory loss can happen, but it is usually limited and improves over time. Your healthcare provider will monitor cognitive function and adjust treatment as needed.
3. Who is a good candidate for ECT?
ECT is typically recommended for individuals with severe or treatment-resistant depression, bipolar disorder, schizophrenia, or catatonia, especially when they don’t respond to other treatments like antidepressant medications or therapy. It’s also used when symptoms are life-threatening and require rapid relief.
4. How many ECT sessions are needed?
A typical course of ECT treatment involves 6 to 12 sessions, administered 2–3 times a week. The exact number varies depending on how the individual responds. Some patients may need long-term or maintenance ECT to prevent relapse, especially in chronic conditions like treatment-resistant depression or bipolar disorder.