Overview of Postpartum Insomnia
Becoming a parent changes nearly every part of daily life, especially sleep. For many new mothers, nights are not only interrupted by feeding and baby care but also by a persistent difficulty falling or staying asleep, even when the baby is sleeping. This condition is known as postpartum insomnia, and it goes beyond ordinary sleep deprivation.
This guide explains what postpartum insomnia is, why it matters for mental health, and how to begin improving sleep with practical, evidence-based strategies that fit real life after birth.
Postpartum insomnia refers to ongoing trouble sleeping after childbirth. This can include:
- Difficulty falling asleep
- Waking frequently during the night
- Trouble staying asleep or falling back asleep
- Lying awake despite extreme exhaustion
Unlike normal newborn-related sleep disruption, postpartum insomnia often continues even when the baby sleeps. Many parents assume this is something they must simply endure, but persistent insomnia after birth is a treatable condition.
How Common It Is and What It Looks Like
Postpartum insomnia is common, especially in the first months after delivery. Typical symptoms include:
- Racing thoughts at bedtime
- Prolonged time falling asleep
- Frequent nighttime awakenings
- Waking too early and being unable to fall back asleep
- Daytime fatigue, irritability, or brain fog
Insomnia after childbirth often overlaps with postpartum depression, anxiety, or heightened stress. When sleep deprivation combines with mood symptoms, recovery can feel much harder without targeted support.
Why Addressing Postpartum Insomnia Matters
Sleep plays a critical role in physical healing, emotional regulation, and cognitive function. Ongoing lack of sleep can:
- Worsen mood and anxiety
- Reduce concentration and memory
- Increase irritability and emotional overwhelm
- Make daily caregiving and self-care more difficult
Distinguishing normal newborn sleep disruption from postpartum insomnia is important. When difficulty sleeping becomes persistent or severe, it signals that additional support may be needed.
When to Pay Closer Attention
You may want to seek help if:
- Insomnia lasts longer than a few weeks
- Sleep loss interferes with daytime functioning
- Mood, anxiety, or concentration continues to worsen
- Sleep feels unmanageable despite basic sleep hygiene changes
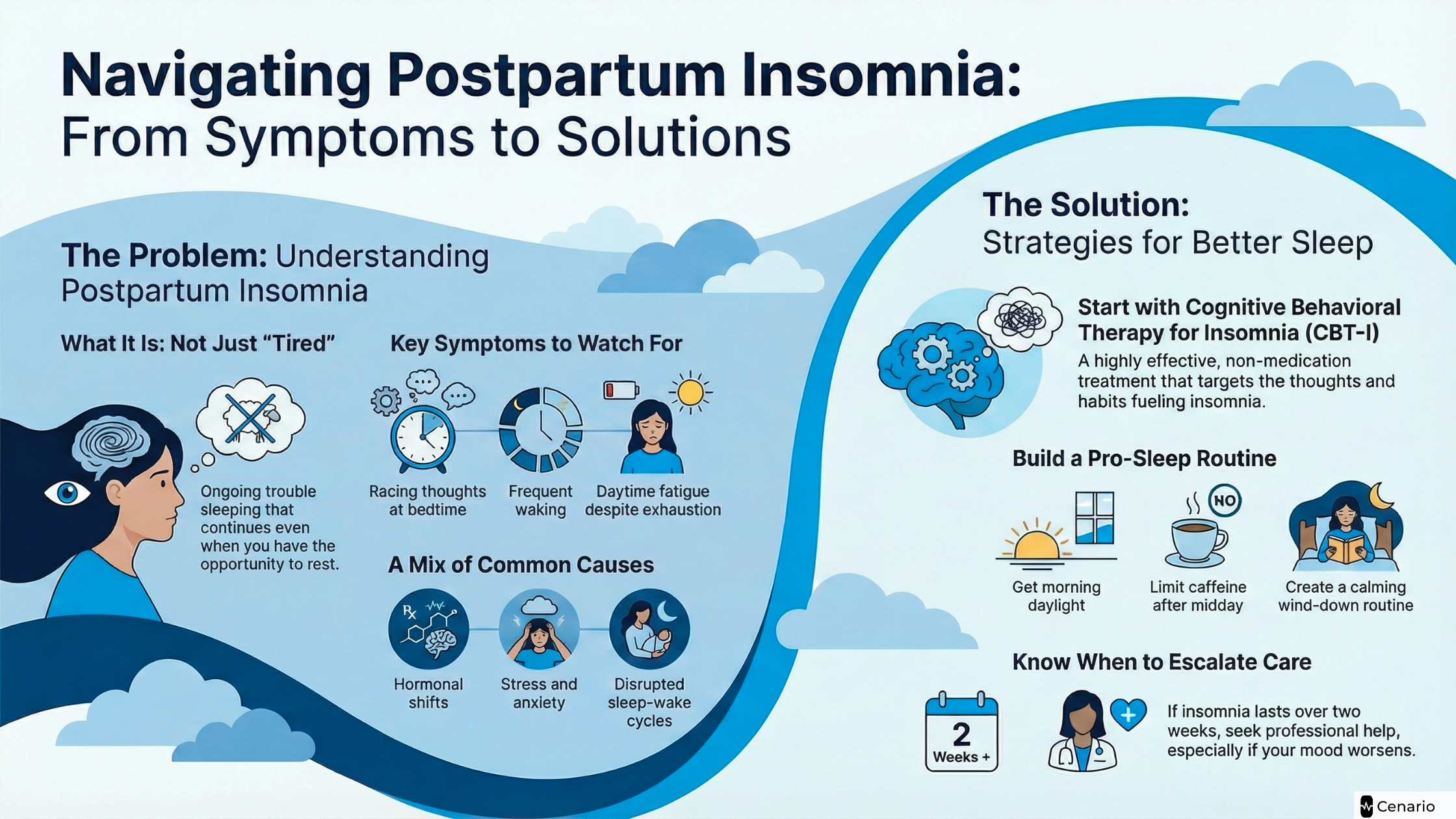
Causes of Postpartum Insomnia
Postpartum insomnia rarely has just one cause. It usually develops from a combination of biological, psychological, and lifestyle factors.
Hormonal Shifts
After birth, estrogen and progesterone levels drop rapidly. These changes can disrupt the circadian rhythm and alter sleep architecture, making it harder to fall or stay asleep.
Night-Time Care and Feeding
Irregular sleep schedules, frequent feedings, and being “on call” overnight interrupt the body’s natural sleep-wake cycle.
Stress, Anxiety, and Mood Disorders
Worry about the baby, racing thoughts, and symptoms of postpartum depression or anxiety often delay sleep onset and increase nighttime awakenings.
Physical Recovery and Discomfort
Pain, surgical recovery, breastfeeding soreness, and physical tension can all interfere with restful sleep.
Circadian Misalignment
Bright light exposure at night and insufficient daytime light can shift the body clock, worsening insomnia.
Co-Occurring Sleep Conditions
Conditions such as restless legs syndrome or sleep apnea may appear or worsen after childbirth, compounding difficulty sleeping.
Evidence-Based Treatments for Postpartum Insomnia
Research consistently shows that behavioral and circadian treatments are the most effective first-line options. Medication may be considered when symptoms are severe and used under medical supervision.
Cognitive Behavioral Therapy for Insomnia (CBT-I)
CBT-I is one of the most effective treatments for insomnia. It targets the thoughts and habits that keep insomnia going.
CBT-I typically includes:
- Sleep education
- Stimulus control
- Sleep restriction techniques
- Strategies to manage nighttime worry
Studies show that CBT-I improves sleep quality and daytime function, with benefits that often last long-term. Programs are available in short, remote, or group formats that fit new-parent schedules.
Learn more on our CBT-I resource page.
Light Therapy and Circadian Support
Timed exposure to bright light in the morning, paired with reduced light at night, helps reset the circadian rhythm. This approach is especially helpful when sleep timing is delayed or when low mood is present.
Simple routines and portable light devices make light therapy practical for parents. Explore options through Cenario’s light therapy resources.
Medications and Breastfeeding Safety
When insomnia is severe or persistent, short-term medication may be part of a treatment plan. Options can include sedative-hypnotics or melatonin supplements.
Safety varies during breastfeeding. Always discuss timing, dosage, and risks with both your prescribing clinician and a lactation consultant before using medication for postpartum insomnia.
Lifestyle and Sleep Hygiene Tips
Small, targeted changes can support better sleep when paired with treatment:
- Keep a consistent sleep window when possible
- Limit caffeine after midday
- Avoid screens at least 30 minutes before bedtime
- Create a short wind-down routine with dim lights and calming activities
- Use naps strategically (20–30 minutes maximum)
- Get daylight exposure and gentle movement during the day
- Ask for help—one uninterrupted sleep block per week can significantly reduce sleep deprivation
Night-Time Care Planning and Trade-Offs
Clear planning reduces stress during difficult nights. Consider these common approaches:
Shared Shifts
One caregiver takes a block of night duty.
Benefit: Longer uninterrupted sleep
Trade-off: Requires coordination and partner recovery time
Pump and Share Feeds
Pumping allows another caregiver to handle night feeds.
Benefit: Longer sleep for the breastfeeding parent
Trade-off: Time, equipment, and supply management
Split Nights
Caregivers alternate nights on duty.
Benefit: Predictable recovery periods
Trade-off: Fewer full nights of sleep overall
Solo Nights
When caring alone, plan short naps, calming routines, and lower daytime expectations.
If-Then Action Plan
Use this simple escalation path:
- If you have several nights of poor sleep with daytime impairment, start a sleep diary
- If insomnia lasts two weeks despite hygiene changes, begin CBT-I or circadian strategies
- If mood worsens, concentration declines, or thoughts of self-harm appear, contact your clinician or emergency services immediately
Download the sleep diary and partner conversation template to make decisions easier on tired days.
Final Thoughts
Postpartum insomnia is common, but it is not something you have to live with indefinitely. The goal is not perfect sleep, but predictable, restorative rest that supports mental health and daily functioning.
Start with one change, track patterns, and commit to a short, structured intervention if sleep does not improve. Take the Cenario Quiz to get a personalized supplements recommendation based on your unique needs.
Frequently Asked Questions
Is postpartum insomnia a sign of postpartum depression?
Not always. Postpartum insomnia can occur on its own or alongside postpartum depression. If insomnia comes with persistent low mood or loss of interest, seek professional help.
Can I take sleep medication while breastfeeding?
Some medications may be used short-term, but safety varies. Always consult your clinician and lactation consultant first.
How long does postpartum insomnia last?
For some, it resolves as routines stabilize. For others, it can persist without treatment. Early use of CBT-I or circadian strategies shortens recovery time and prevents chronic insomnia.







