Understanding the Link Between Menstrual Cycles and Insomnia
Many people who menstruate notice that their sleep problems get worse around their period. If you’ve ever felt more tired, irritable, or foggy during this time, you’re not alone. Trouble falling or staying asleep during the menstrual cycle is common, especially in the days leading up to your period (known as the luteal phase) or the first few days of bleeding.
Understanding how hormone fluctuations affect your body, mood, and sleep is the first step to feeling better, and planning ahead.
Understanding the Link Between Menstrual Cycles and Insomnia
Your menstrual cycle impacts more than just your physical symptoms. During the late luteal phase, just before your period starts, your progesterone and estrogen levels drop sharply. These changes can affect:
- Body temperature (making it harder to fall asleep)
- Melatonin production (which helps regulate your sleep)
- Brain chemistry (which influences mood and anxiety)
At the same time, common PMS symptoms like cramps, bloating, or breast tenderness can interrupt your rest. Anxiety, low mood, and stress can make sleep even harder.
Why Insomnia Around Your Period Matters
Poor sleep quality during your cycle affects more than just your energy levels. Even a few bad nights can make it harder to focus, increase mood swings, and reduce your ability to handle daily tasks. People with premenstrual syndrome (PMS) or premenstrual dysphoric disorder (PMDD) often deal with more intense sleep problems, which can interfere with work, school, or relationships.
What You’ll Learn in This Guide
In this article, we’ll explain:
- How hormone changes in your menstrual cycle impact sleep cycles
- Why physical symptoms and mood affect how well you fall asleep and stay asleep
- How to use practical strategies and circadian rhythms to improve your sleep
You’ll also get tracking tips and tools to identify your personal risk window—when you’re most likely to struggle with sleep.
The Science Behind Menstruation and Sleep Problems
Hormonal Fluctuations and Sleep Chemistry
- Progesterone is known for its calming effects. It boosts GABA, a brain chemical that helps you relax. After ovulation, progesterone levels are high, which may help some people sleep. But just before your period, when progesterone drops, sleep becomes lighter and more broken.
- Estrogen plays a role in melatonin and serotonin production. When estrogen levels drop, melatonin falls too, affecting how deeply and how long you sleep.
Brain Chemistry and Mood
When hormones shift, serotonin and GABA levels also change. This can cause anxiety, racing thoughts, and a sense of restlessness before your period. This explains why you may feel more “wired” at night even when you’re exhausted.
Body Temperature and Circadian Rhythms
Normally, your body temperature drops at night to help you sleep. But progesterone increases body heat after ovulation. When it falls right before your period, your temperature rhythm is disrupted, making it harder to fall or stay asleep.
Physical Symptoms That Disrupt Sleep
Pain from cramps, bloating, or headaches can cause micro-awakenings that break up your sleep cycles. This is often linked to prostaglandins, chemicals that trigger pain and inflammation during menstruation.
Mood and Stress Response
Low mood, irritability, and anxiety often spike during PMS. These emotional shifts raise cortisol, your body’s stress hormone, which keeps your brain alert. In turn, poor sleep makes mood symptoms worse, creating a frustrating cycle.
Timing: Why Symptoms Appear in Predictable Patterns
Studies show that sleep disruption usually happens in the late luteal phase and may continue into the early days of menstruation. Knowing when your symptoms peak lets you plan ahead. That’s the power of chronobiology, the science of your internal body clock.
Who’s Most at Risk?
You’re more likely to experience insomnia during your cycle if you have:
- PMS or PMDD
- Chronic period pain (dysmenorrhea)
- Anxiety or depression
- Irregular sleep patterns or shift work
- High caffeine or alcohol use at night
When to Seek Help
If insomnia and menstruation are causing problems in your daily life, talk to a healthcare provider. You may have PMDD, a mood disorder, or a separate sleep condition that needs support. Don’t wait, help is available.
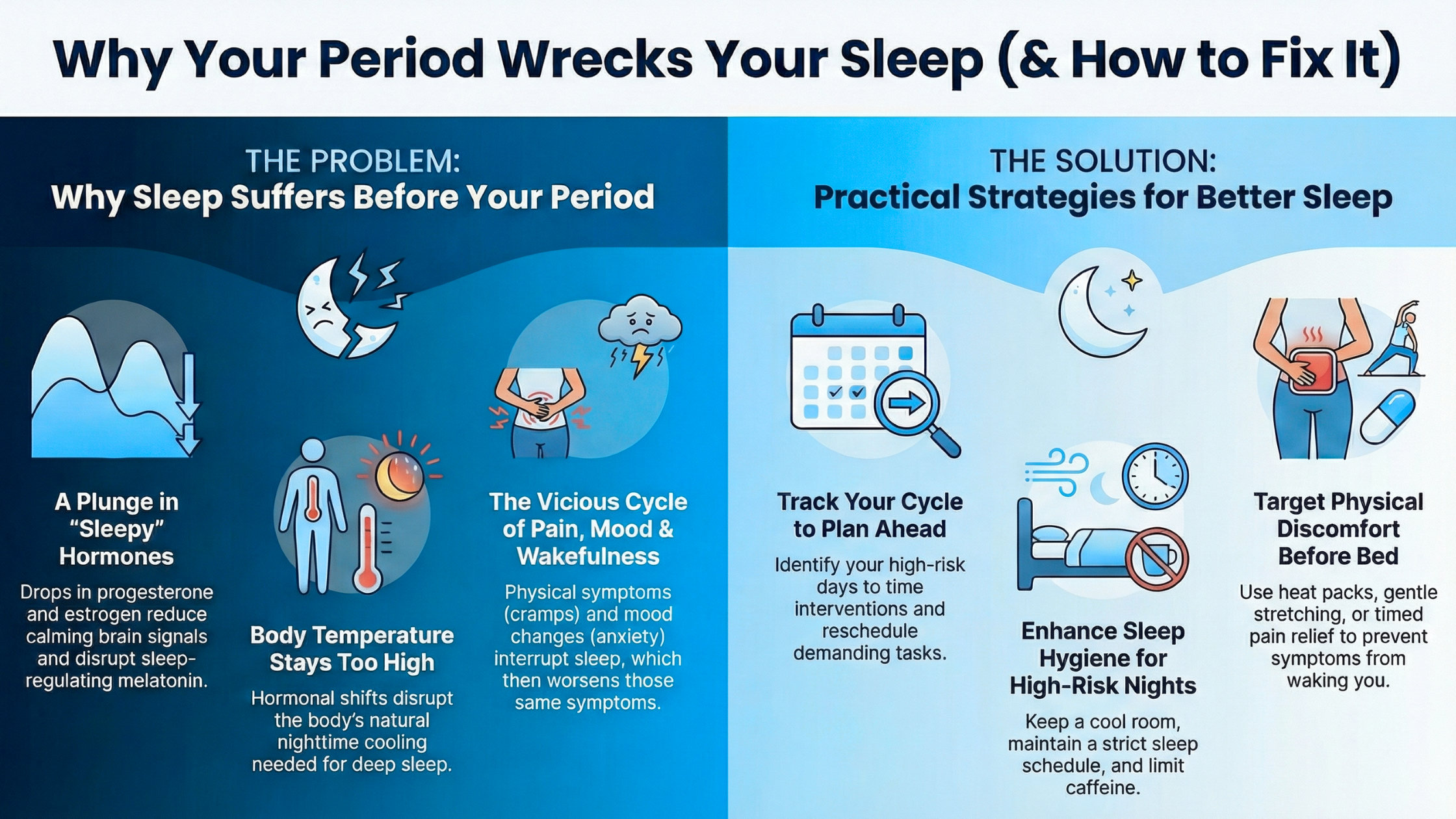
Simple Ways to Improve Your Sleep During Your Cycle
1. Optimize Sleep Hygiene Based on Your Cycle
During the 3–7 days before your period and the first 48 hours of bleeding, try:
- Sticking to the same time every day for sleep and waking
- Lowering your bedroom temperature
- Avoiding caffeine after 2 p.m. and cutting alcohol
- Reducing screen time and using soft, warm light before bed
2. Manage Physical Discomfort
Pain is a major reason for poor sleep quality. You can try:
- Taking pain relief at the right time for best effect
- Using heat packs or gentle yoga stretches before bed
- Eating anti-inflammatory foods in your luteal phase
3. Use CBT-I Techniques
Cognitive Behavioral Therapy for Insomnia (CBT-I) works well for cycle-related insomnia:
- Use your bed only for sleep (not worry)
- Try calming thoughts or breathing techniques before bed
- Avoid harsh sleep restrictions unless poor sleep is constant
4. Track Your Sleep and Cycle Together
Apps or wearables that track menstrual cycles and sleep can help you:
- Avoid scheduling big events during your high-risk days
- Plan relaxing routines and earlier bedtimes before your period
- Experiment with changes like caffeine timing or exercise
5. Try Natural Aids (With Medical Guidance)
- Melatonin (low dose, short-term, and only under supervision)
- Magnesium or herbal supplements (after checking safety)
- Guided relaxation or mindfulness before bed
Planning for Work, School, and Life
When hormone shifts affect your energy and focus:
- Avoid scheduling big tasks during high-risk days
- Tell teammates or teachers if your energy varies
- Use short naps or light workloads after bad nights
Final Thoughts: Make Your Cycle Work for You
Your sleep doesn’t have to suffer every month. By understanding how estrogen and progesterone impact your rest, you can take simple, proactive steps to feel more in control of your nights, especially during the toughest parts of your menstrual cycle.
Begin by tracking your PMS symptoms and sleep patterns for two to three cycles. As you start to notice patterns, introduce one or two new sleep strategies during your luteal phase, such as better sleep hygiene, targeted pain relief, or mindfulness before bed. Give your body time to respond, and adjust your approach based on what works for you.
If you’re still struggling with poor sleep or suspect you may have PMDD or other health concerns, don’t hesitate to consult a clinician for professional support.
Want personalized support? Take the Cenario Quiz to get customized supplement recommendations designed to support your unique cycle, mood, and sleep needs.
Frequently Asked Questions
How do hormone changes during the menstrual cycle affect sleep?
Drops in estrogen and progesterone during the luteal phase can disrupt sleep cycles by affecting melatonin production, raising body temperature, and increasing anxiety. These changes make it harder to fall asleep and stay asleep, especially in the days before your period.
What’s the difference between PMS and PMDD in terms of sleep?
PMS may cause mild sleep problems, while PMDD leads to severe insomnia, anxiety, and mood swings that disrupt daily life. People with PMDD often struggle to sleep during the late luteal phase and feel better once menstruation begins. If symptoms are intense, seek medical support.
Can cycle tracking really help improve my sleep?
Yes. Tracking your menstrual cycle and PMS symptoms helps you predict when sleep issues are most likely. With this info, you can plan sleep strategies in advance. For personalized support, take the Cenario Quiz to get custom supplement recommendations based on your cycle..
.







